Hyperbaric Oxygen Therapy in Wound Healing
Joseph Priestley discovered Oxygen in 1775. Little did he knew that a gas considered toxic due to its effect on CNS and Lungs would be used therapeutically in near future!
Hyperbaric Oxygen Therapy has been used in management of air and gas emboli, decompression sickness, Carbon monoxide poisoning, wound management and may other medical conditions. We will discuss the mechanisms through which it works in the management of above cases while specifically discussing about its mechanisms in wound healing.
Hyperbaric Oxygen Therapy – General Mechanisms
So, whenever we think about how Hyperbaric oxygen might work, it immediately clicks in our mind that hyperbaric Oxygen is just Oxygen gas at high pressures, and it will mechanically compress the gases which are present in our bloodstream and probably this might be its mechanism of action.
However it is not as simple as it looks !
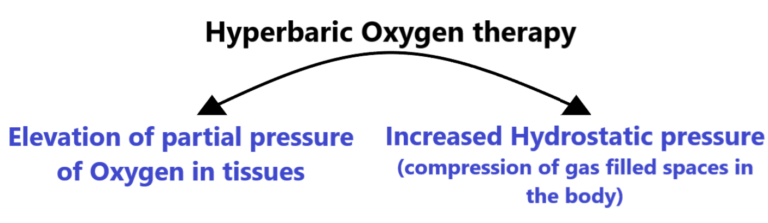
The two aspects of Hyperbaric Oxygen contribute to its therapeutic action –
- The elevated partial pressure of inspired O2, and
- Increased Hydrostatic pressure throughout the body present in the HBOT chamber.
Let’s discuss them one by one –
1. The elevated partial pressure of Inspired O2
When the subject breathes 100% O2 at elevated pressures (usually 3 atm), more amount of O2 diffuses into the blood owing to a large pressure difference along the alveoli. It has been estimated that there is a net increase of dissolved O2 by 22.7%. This creates a state of excess O2 in the blood known as Hyperoxia. This O2 now goes to mitochondria to serve as the final electron acceptor in the electron transport chain. During this process a lot of free radicals are generated. In this way hyperoxia increases the production of reactive O2 species (ROS) and Reactive nitrogen species (RNS).
But wait! This doesn’t seem to be going in the right path. One might wonder that the ROS & RNS generated due to hyperoxia would cause more damage than good.
So here comes the interesting part. HBOT is not given continuously, rather a typical HBOT session varies from 1.5 to 2 h and is usually performed from one to three times daily, being given among 20 to 60 therapeutical doses depending on the medical condition. Thus, HBOT generates hyperoxia intermittently and this intermittent hyperoxia causes a transient rise of ROS & RNS, and to our surprise, this transient rise causes many beneficial effects including the synthesis of different growth factors finally improving neovascularization and immunomodulatory properties. This property is called Hormesis.
2. Increased Hydrostatic pressure throughout the body
Now let’s revisit one of the laws we’ve read in our +2s – ‘The Henry’s Law‘. It states that the amount of gas that is dissolved in a liquid is directly proportional to the partial pressure of that gas above the liquid when the temperature is kept constant.
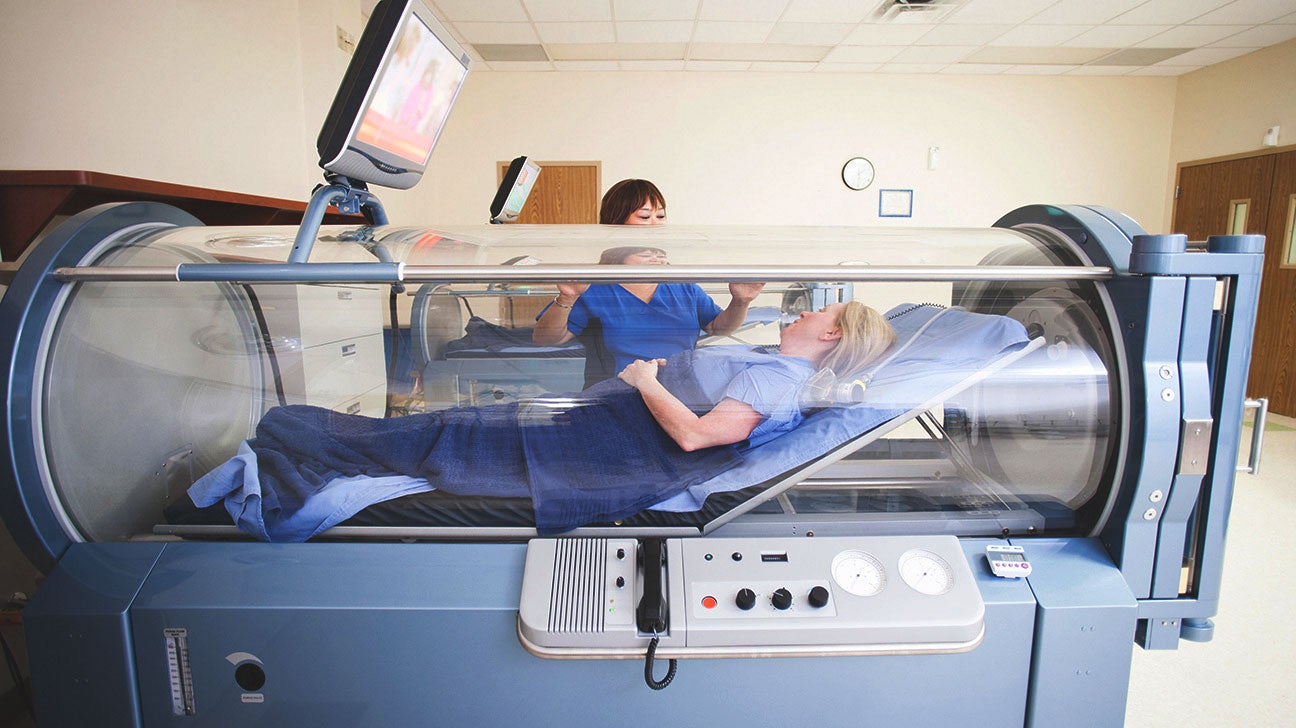
For administration of the therapy the patient is taken to a specially designed chamber and the pressure inside the chamber is set to almost 1.5-3 times the normal air pressure. At this moment the patient is inside the chamber and every tissue including blood inside his/her body is experiencing increased pressure.
Our blood contains gases which are circulating in a dissolved form. So, this increased pressure contributes to a compression of all gas-filled spaces in the body (Henry’s Law) and is relevant to treat conditions where gas bubbles are present in the body and cause the disease (e.g. intravascular embolism; decompression sickness with intravascular or intra-tissue bubbles).
Hyperbaric Oxygen Therapy – Specific Mechanisms
Hyperbaric Oxygen Therapy in Wound healing
HBOT plays a major role in wound healing and is nowadays indicated for microbial-infected wounds (e.g., Clostridial myonecrosis and Fournier’s gangrene), traumatic wounds, thermal burns, skin grafts, radiation-induced wounds & diabetic and vascular insufficiency ulcers.

Role of Oxygen
Oxygen is required for healing in multiple ways –
- Oxygen is required for adenosine tri-phosphate synthesis within the mitochondria (through complex V of Electron transport chain) for oxidative metabolism.
- essential for collagen and protein synthesis.
- Oxygen acts as cofactor for enzymes which synthesize collagen & protein. For eg – Mature collagen synthesis requires prolyl-hydroxylase and lysyl-hydroxylase, which are enzymes dependent on oxygen for function.
Oxygen is a substrate for all NOX enzymes(NADPH oxidases), which are a major source of ROS. The production of ROS during wound healing is critical for cell signaling, angiogenesis, and wound disinfection.
- NO is produced by the nitric oxide synthase (NOS) family of enzymes, which require molecular oxygen as a co-substrate for the oxidation of the amino acid L-arginine to NO and citrulline. NO plays a critical role in the regulation of vascular tone and angiogenesis in the wound bed.
Increase in NRF2
NRF2 stands for Nuclear factor erythroid 2-related factor 2, it is a transcription factor which regulates the expression of antioxidant proteins that protects the cell against oxidative damage triggered by injury and inflammation.
Wounded tissues normally produce large amounts of ROS to combat invading pathogens, to attract immune cells, and to regulate different cell signaling events and this process is aided by high partial pressures of O2. ROS and other electrophilic compounds induce the activity of NRF2 by stabilizing it and regulating its degradation. NRF2 regulates the transcription of cytoprotective genes, including genes encoding various ROS-detoxifying enzymes, antioxidant proteins, and drug transporters by binding to antioxidant response elements (AREs) in the promoter regions of genes encoding cytoprotective proteins.
Epithelialization and Neovascularization
Hyperbaric Oxygen promotes epithelization and neovascularization through up-regulation of host factors like tumor necrosis factor-α (TNF-α), matrix metallopeptidase 9 (MMP-9) and tissue inhibitor of metalloproteinase-1 (TIMP-1).
Hyperbaric Oxygen Therapy in Infections
THE HYPOXIA-HYPEROXIA PARADOX
The actions of Hyperbaric oxygen therapy i.e. exposure of cells to intermittent hyperoxic environment, induces mediators and cellular adaptive mechanisms which are similar to those induced by hypoxia.
- HBOT upregulates HIF that induces the expression of Nitric Oxide Synthases (NOS) and virus killing peptides (defensins and cathelicidins such as cathelin-related antimicrobial peptide) with consequent neutrophil and monocyte phagocytosis of the microbes.
- Cathelicidin peptides are dual-natured molecules called amphiphiles: one end of the molecule is attracted to water and repelled by fats and proteins, and the other end is attracted to fat and proteins and repelled by water. Members of this family react to pathogens by disintegrating, damaging, or puncturing cell membranes.
- Anaerobic bacteria are killed by a much higher amount of pressurized O2 (bacteriostasis)
- Anti inflammatory potential – prevents rolling and activation of WBCs –prevents reperfusion injuries.
- Intracranial abscess (ICA)
- Inflammatory response may damage the surrounding brain parenchyma causing morbidity and mortality. Infection proper and the use of antibiotics leads to a localized acidotic and hypoxic environment. HBOT impairs the acidotic and hypoxic environment in ICAs due to the proper infection and the use of antibiotics.HBOT being a non-invasive and safely tolerated method, is accepted as an adjunctive therapy in patients suffering from ICA.
- osteomyelitis
- Osteomyelitis becomes a challenging condition to treat, as many antimicrobials do not penetrate in the bone properly. HBOT acts as a synergist to antibiotic activity, while enhancing angiogenesis, leukocyte oxidative killing and osteogenetic process.
- HBOT upregulates HIF that induces the expression of Nitric Oxide Synthases (NOS) and virus killing peptides (defensins and cathelicidins such as cathelin-related antimicrobial peptide) with consequent neutrophil and monocyte phagocytosis of the microbes.
Hyperbaric Oxygen Therapy in Medical Emergencies
Decompression Sickness & Air embolism
Central retinal artery occlusion (CRAO)
CRAO is an ophthalmological complication caused by a permanent occlusion of the central retinal artery, mostly due to an embolus at its narrowest part that is typically associated with a sudden, massive loss of vision in the affected eye. It should be noted that retinal tissue has the highest Oxygen consumption rate in the body, which makes it nontolerant to hypoxia.
Hyperbaric oxygen therapy helps in providing more oxygen to the tissues and thus minimizes the ischemic damage to the retina.
Trauma & Crush injuries
The affected tissue suffer from hypoxia, edema and ischemia & HBOT improves neovascularisation and promotes healing.
Carbon monoxide poisoning
CO is readily absorbed through the lungs and binds to the hemoglobin molecule in red blood cells with an affinity 240 times that of oxygen. The COHb thus formed, impairs the delivery of the remaining oxygen bound to the hemoglobin molecule. This results in decreased oxygen delivery to the tissues and relative tissue hypoxia.
Not only this, almost 10% to 15% of the CO binds to myoglobin, cytochromes, and NADPH reductase, thus impairing oxidative phosphorylation in the mitochondria of the cells. This is especially toxic to the heart muscle and the brain, as they have high oxygen demands. This results in the classic symptoms of headache, dizziness, nausea, vomiting, flu-like symptoms, fatigue, shortness of breath, impaired judgment, and cognitive dysfunction, chest pain, agitation, abdominal pain, drowsiness, loss of consciousness, visual changes, and seizures.
CO is itself toxic and damages the endothelial cells of the vessels in the brain. Neutrophils adhere to these damaged endothelial cells. Activated neutrophils release an enzyme called as Xanthine oxidase which generates Oxygen Free radicals and is thus responsible for the cytotoxic property of neutrophils.
Lipid peroxidation by toxic oxygen species generated by xanthine oxidase in the brain cause neurological sequelae such as depression, memory problems, ataxia, behavior problems, and impaired cognitive function.
Hyperbaric Oxygen competitively binds with haemoglobin & rapidly displaces CO from Hb and generates normal oxyhemoglobin in the red blood cell. Hyperbaric oxygen therapy reduces the adherence of neutrophils on the damaged endothelium of the blood vessels in the brain, which reduces tissue edema and reduces lipid peroxidation. The extra oxygen that is delivered to the tissue also helps to reduce the CO bound to the cytochrome proteins in the mitochondria of the cells and contributes to restoring oxidative phosphorylation, which neurons are especially dependent upon for normal function and survival from the ischemic insult. It also decreases the risk for brain injury and nerve damage(delayed neuropsychiatric syndrome) through its anti-inflammatory properties.
Anaemia
As Hb levels drops to a critical level, O2 delivery to the tissues gets impaired. In this line, the use of 100%, hyperbaric O2 solves the problem by increasing the amount of oxygen dissolved in the plasma by virtue of the Henry’s Law.
Sensorineural Hearing Loss (SNHL)
Sudden sensorineural hearing loss (SSNHL) is defined as hearing loss of at least 30 decibels occurring over at least three consecutive audiometric frequencies and lasting for at least 3 days.
Hearing function in the inner ear is maintained by the cochlea which has a high oxygen demand. Cochlear hypoxia is associated with progressive ossification, fibrosis, loss of neurons, endolymphatic hydrops, and hearing loss. Direct blood supply to the organ of Corti is minimal, so oxygen must diffuse through the perilymph and cortilymph.
The labyrinthine artery (internal auditory artery) is a long, slender branch of the anterior inferior cerebellar artery or the basilar artery. It accompanies the vestibulocochlear nerve through the internal acoustic meatus into the inner ear. Labyrinthine artery occlusion has shown to cause progressive degenerative changes, fibrosis, new bone formation, and hearing loss. Any pathology that results in vascular occlusion of this artery can result in hearing loss.
HBOT not only prevents Cochlear hypoxia by increasing the amount of Oxygen delivery but also helps in resolving vascular occlusion in the labyrinthine artery if any. Also, HBOT protects the hair cell stereocilia, through hormetic mechanisms. Hormesis is a biological phenomenon where a low dose of a potentially harmful stressor, such as a toxin or environmental factor, stimulates a beneficial adaptive response in an organism. In other words, small doses of stressors that would be damaging in larger amounts can actually enhance resilience, stimulate growth, or improve health at lower levels.
Femoral head necrosis
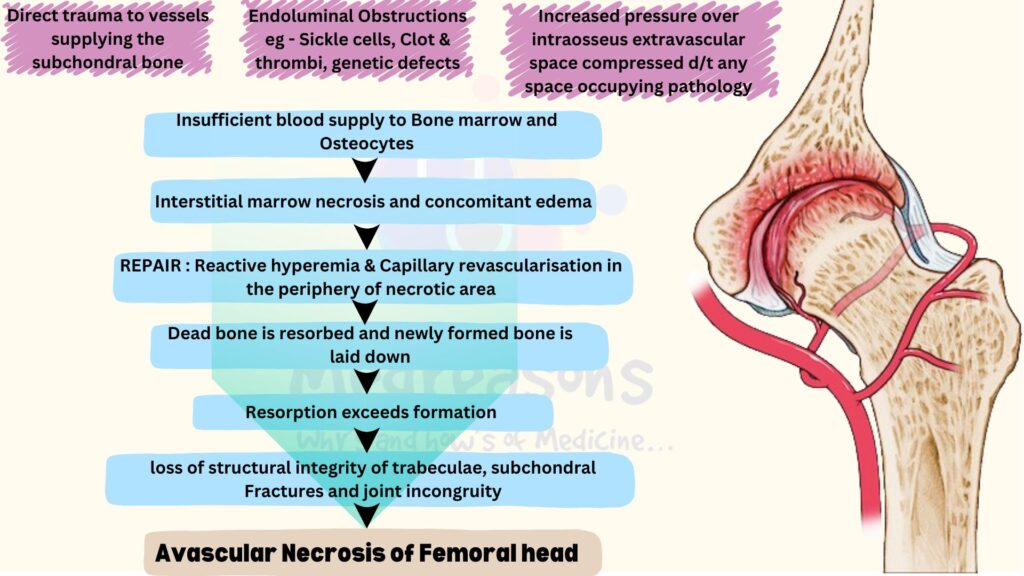
Femoral Head necrosis also called as Avascular necrosis of the femoral head, is mainly caused by a compromised blood supply to the bone ultimately leading to apoptosis of bone marrow cells and osteocytes.
Hyperbaric Oxygen therapy works by promoting neo angiogenesis and neovascularization, by increasing extracellular oxygen concentration, by reducing cellular ischemia and edema by causing vasoconstriction, and by reducing bone marrow pressure and improves oxygen delivery to ischemic cells, thus preventing further necrosis.
